Wisdom teeth, also known as third molars, are the final set of teeth to emerge in the mouth. While some individuals experience no issues with their wisdom teeth, many face complications due to lack of space or misalignment. As a result, wisdom teeth removal becomes necessary to prevent pain, infection, and potential damage to surrounding teeth. Process of wisdom teeth removal, its importance, and what to expect during and after the procedure.
Smooth Recovery Essential Tips for Healing After Wisdom Teeth Extraction
Wisdom teeth typically start to emerge in the late teens or early twenties when the jaw is fully developed. However, due to limited space in the mouth, these molars often don’t have enough room to grow properly. This can lead to various problems, including impaction (when the tooth is trapped beneath the gum line), crowding, shifting of neighboring teeth, infections, and even cysts or tumors. Wisdom teeth removal is a common dental procedure performed by oral surgeons or dentists experienced in oral surgery. The goal is to extract problematic wisdom teeth to alleviate pain, prevent complications, and maintain optimal oral health. During the wisdom teeth removal procedure, local or general anesthesia is administered to ensure the patient’s comfort. The oral surgeon makes an incision in the gum tissue, exposes the tooth, and may need to remove any bone obstructing the tooth’s access. The tooth is then carefully extracted, and the site is sutured if necessary.
Anatomy, Function, and Common Problems
Wisdom teeth, also known as third molars, are the last set of teeth to develop in the mouth. They typically appear between the ages of 17 and 25, a time commonly referred to as the “age of wisdom.” However, due to evolutionary changes and dietary shifts, many individuals no longer have enough space in their jaws to accommodate these additional teeth. Wisdom teeth serve little to no functional purpose in modern humans. Our ancestors relied on these molars to chew tough and coarse foods, but with advancements in diet and oral hygiene, the need for wisdom teeth has diminished. As a result, they often become problematic when they attempt to erupt.
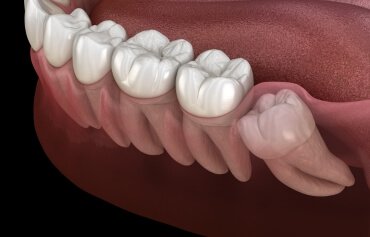
Signs and Symptoms of Problematic Wisdom Teeth
Not all wisdom teeth cause problems, but when they do, the signs and symptoms can be quite apparent. Common indicators of problematic wisdom teeth include:
Pain or discomfort in the back of the mouth
Swelling and inflammation of the gums
Jaw stiffness or difficulty opening the mouth.
Redness and tenderness around the wisdom tooth area
Bad breath or an unpleasant taste in the mouth
Crowding or shifting of adjacent teeth
These symptoms can be indicative of various issues, such as impact (when the tooth is trapped beneath the gum line), infection, decay, or cyst formation. When these problems arise, it is crucial to consider wisdom teeth removal as a preventive measure to avoid further complications.
The Wisdom Teeth Removal Process
Before undergoing wisdom teeth removal, a thorough examination is conducted by a dental professional. This typically involves dental X-rays to assess the position and condition of the wisdom teeth. Based on the findings, the dentist or oral surgeon will determine the necessity and timing of the extraction. During the preparation phase, the dentist will discuss the procedure, explain any risks or potential complications, and address any concerns or questions the patient may have. Pre-operative instructions, such as fasting requirements and medications to avoid, will be provided.
Anesthesia Options for Wisdom Teeth Extraction
To ensure a comfortable experience during the wisdom teeth removal procedure, anesthesia options are available. Local anesthesia is commonly used to numb the area surrounding the wisdom teeth, providing pain relief during the extraction. It allows the patient to remain awake but not feel any pain or discomfort. In some cases, intravenous sedation or general anesthesia may be recommended, particularly for complex or multiple extractions or for patients with dental anxiety. The dental professional will discuss the anesthesia options and help determine the most suitable choice based on the patient’s medical history, procedure complexity, and personal preferences.
What to Expect During Wisdom Teeth Removal
The actual process of wisdom teeth removal involves several steps. The dentist or oral surgeon will make an incision in the gum tissue to expose the tooth and may need to remove a small amount of bone if necessary. The tooth is then gently rocked back and forth to loosen it from the surrounding ligaments and socket before being extracted. In some cases, the tooth may be sectioned into smaller pieces for easier removal. Once the tooth is fully extracted, any necessary sutures are placed to promote proper healing. The length of the procedure can vary depending on the complexity of the extraction and the number of teeth being removed. Patients will be closely monitored throughout the process to ensure their safety and comfort.
Surgical vs. Non-Surgical Wisdom Teeth Removal
When it comes to wisdom teeth removal, there are two primary approaches: surgical and non-surgical. The choice between the two depends on various factors, including the position, condition, and complexity of the wisdom teeth, as well as the individual’s overall oral health. Understanding the differences between surgical and non-surgical wisdom teeth removal can help patients make an informed decision and have a better understanding of what to expect during the procedure. Non-surgical wisdom teeth removal, also known as simple extraction, is typically performed when the wisdom teeth have fully erupted and are positioned properly in the mouth. In this procedure, the dentist or oral surgeon numbs the area with local anesthesia and uses dental instruments to loosen and remove the tooth. The recovery time for non-surgical extraction is generally faster, and patients can often resume their normal activities within a few days. On the other hand, surgical wisdom teeth removal is necessary when the teeth are impacted or partially erupted, meaning they have not fully emerged through the gum line. Surgical extraction may also be required if the wisdom teeth are positioned in a way that makes them difficult to access or if they are causing complications such as damage to neighboring teeth or infections. This procedure is more complex and may require the use of general anesthesia or intravenous sedation to ensure the patient’s comfort. Surgical removal involves making an incision in the gum tissue, removing any bone that obstructs the tooth, and extracting the tooth in sections if necessary. The recovery period for surgical extraction is typically longer, and patients may experience more swelling and discomfort during the healing process.
